The TSW debate: Review the research and decide for yourself

There is some debate as to whether Topical Steroid Withdrawal (TSW), Red Skin Syndrome and Steroid Addiction exists.
People claim to have it, many doctors say there is no scientific proof.
This page contains a list of scientific papers and reviews discussing topical steroid withdrawal, red skin syndrome and steroid addiction, with direct links to the research papers.
Please come to your own conclusions. This is (mostly) not an opinion piece, apart from my personal wish in the next paragraph which explains my reason for compiling this research. If you are a health practitioner and would like a TSW research page free from comment (to pass on to others), view our comment-free version of this article here.
{my wish}
TSW can be a highly depressing period in a person's life, and support is an important part of a person's recovery. However, a common complaint from those going through TSW is when doctors and dermatologists tell them there is no evidence that TSW exists. Some even roll their eyes when the patient mentions TSW.
We hope patients and health practitioners find this resource page useful so they can communicate more effectively, and with compassion and understanding.
Please note I am not against the short term use of topical steroids, which I have outlined in my other articles and I will not cover it again here. I am pro choice, and only you can decide what is right for you.
Note there are doctors who believe in TSW and you can find examples of them in the following research articles.
To skip to the research articles, click on 'TSW Research', below, or continue to read as I briefly discuss TSW and rosacea.
What is TSW?
Topical Steroid Withdrawal (TSW for short) is the cessation of applying topical steroids to the skin, after using them for a period of time AND then experiencing significant, visible withdrawal symptoms. The resulting condition is often called Red Skin Syndrome.
Not all people who have applied topical steroids (short term or long term) experience TSW. For example, I used topical steroids for years as a teenager and beyond, and I ended up with mild thinned skin on my face (not TSW). But other people have had a different experience to my own.
Note I do not recommend you suddenly stop using topical steroids if you are currently using them (see my other other blog articles to find out why).
Is TSW actually rosacea?
After more than 15 years of working almost exclusively with eczema and skin rash patients, I noticed that some patients had a type of eczema that was redder, it had a strong smell and it mimicked rosacea. So I thought hey that's eczema AND rosacea. I think a lot of health practitioners presume this too.
However, people with rosacea don't have elephant skin (where the arms, knees and/or legs have deep folds of skin), and the don't generally peel from head-to-toe, they don't spend all day lying in a bath to get some relief. People with rosacea don't wake up in the morning with their bed covered in visible pools of skin flakes. But people with TSW say they do.
TSW is not rosacea, but at first glance it looks A LOT like it.
So does TSW (red skin syndrome) really exist?
Here is a list of scientific papers about TSW for patients and health practitioners to read.
We hope this helps to bridge the communication gap between patients and health practitioners.
Each article has a link so you can read the research for yourself:
TSW Research
1. 'Steroid Addiction', International Journal of Dermatology, 1979

This review from the University of Pennsylvania School of Medicine (US), and the University of Munster School of Medicine, in West Germany, was published in 1979. Read 'Steroid Addiction' here.
2. 'The red skin syndromes: corticosteroid addiction and withdrawal', Expert Review of Dermatology, 2006
This abstract from the 'Expert Review in Dermatology' discusses 1500 patients who were treated and evaluated. Read the research paper here
3. 'Adverse effects of topical glucocorticosteroids', Journal of the American Academy of Dermatology, 2006
This research paper discusses the significant milestone corticosteroids have had in the practise of dermatologic therapy. It discusses how the clinical practise of reporting adverse drug reactions is poor despite encouragement to do so. Read the research paper here.
4. 'Side effects of topical steroids' - a long overdue visit, Indian Dermatology Online Journal, 2014
The ‘Indian Dermatology Online Journal’ brings attention to the effectiveness of topical steroids and the misuse of these creams which can lead to systemic and psychological side effects, which are discussed in detail. Read the research paper here.
5. 'A systematic review of topical corticosteroid withdrawal in patients with atopic dermatitis and other dermatoses', American Academy of Dermatology, 2015
This review was reported by ‘The American Academy of Dermatology’, due to the increasing number of patient’s enquiries to the National Eczema Association regarding steroid addiction syndrome. Read the research paper here.
6. 'Topical steroid addiction in atopic dermatitis', Drug, Healthcare and Patient Safety, 2014
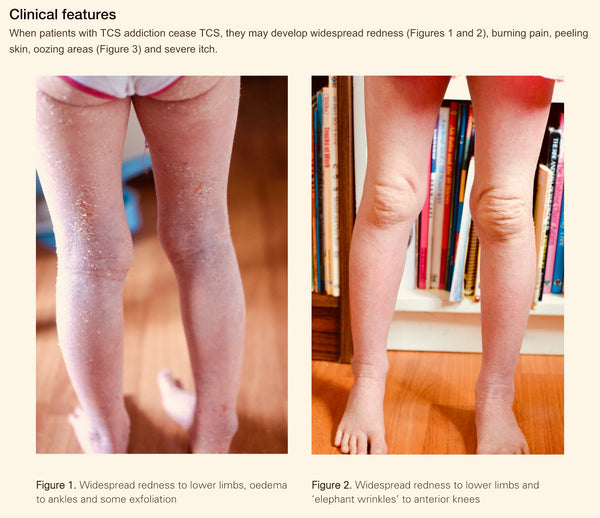
This article addresses the clinical features of topical steroid addiction. The aim of this article is to help explain this illness and spur the discussion of TSW and red skin syndrome. Images are included. Read the research paper here.
7. 'Prevalence of atopic diseases and the use of topical corticosteroids - is there a connection?', Medical Hypotheses, 2005

Read the article here.
8. 'Serum nitric oxide levels in red patients - separating corticosteroid -addicted patients from those with chronic eczema', Jama Dermatology, 2004
This article discusses the difference between chronic eczema and patients addicted to topical steroids.
The article concludes by saying, "we believe that the rash does not represent eczema anymore but permanent vasodilation caused by elevated serum levels of nitric oxide.
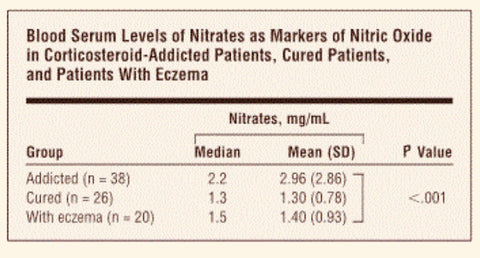
Read research paper here.
9. 'Corticosteroid addiction and withdrawal in the atopic: the red burning skin syndrome, Clinics in Dermatology, 2003
This report was conducted by researchers from the Department of Dermatology, UCLA School of Medicine, Los Angeles. It shows graphic photos and descriptions of different cases. The pattern of topical steroid withdrawal is described in detail.
Warning: this research paper contains graphic images and is not suitable for viewing if you are under 18. Read the research paper here.
10. 'Topical steroid addiction and withdrawal - an overview for GPs', Australian Family Physician, Ear, Nose and Throat, 2016
This is an interesting article written by Dr. Belinda Sheary from the Royal Randwick Medical Centre, Randwick, Australia. Also see her research paper, below (No. 12). Read the article here.
11. 'Topical corticosteroid-induced rosacea-like dermatitis: A clinical study of 110 cases', Indian Journal of Dermatology, 2011.
This article discusses the "rosacea-like" appearance of dermatitis which can occur after prolonged and continuous use of topical steroids. Read the research paper here.
12. 'Steroid Withdrawal Effects Following Long-term Topical Corticosteroid Use', Dermatitis, 2018.
Australian doctor Belinda Sheary, recently published this TSW article in the journal Dermatitis. Dr Belinda Sheary is an Australian GP with a special interest in Topical Steroid Withdrawal. Her general practice is in Randwick, Sydney. Read the research here.
Our eczema patients who see us for nutritional programs and advice often ask us to recommend supportive doctors who believe in TSW. If you are a registered doctor who fits this description, let us know and we can add you to a resource page to give to our patients.
What if you want to stop applying topical steroids?
It's not my intention to convince people to suddenly stop using topical steroids, as TSW can sometimes occur. And it's not pleasant. It can take time to recover so you need to be prepared.
If you are considering going off topical steroids read this article first as it explains why you should do this slowly, not suddenly. Also find a supportive doctor to help you along the way.
Other medical options:
I have spoken with doctors who recommend switching from topical steroids to immunosuppressants to help ease the symptoms when ceasing topical steroids after extended use. While swapping one drug for another is not ideal, it is an option for those who have severe adverse reactions after stopping the steroids. It's important to have choices which is why I am mentioning this option. Speak with a supportive doctor for more advice.
BE healthy
Meditate. Eat well. For 17 years I have recommend 'low chemical' diets for eczema, plus food intolerance diagnosis, as chemical sensitivity and food intolerances are often involved in the appearance of eczema. Do the investigation work to find our all your triggers, and then avoid them.
For more TSW and eczema articles, wander around our website or see my products here.
***
Article by nutritionist Karen Fischer, author of The Eczema Diet and The Eczema Detox; research compiled by nutritionist Katie Layland and Karen Fischer, 12 July 2018. Food images by Karen Fischer; food preparation by Katie Layland. Recipe available for members of Karen's newsletter.
How to quote: Fischer, K., 2018, 'Does TSW exist? Review the research and decide for yourself', Eczema Life Clinic, Sydney, Australia.
Products
At Eczema Life, we recommend nutritionist Karen Fischer's low food chemical program (The Eczema Detox) along with additive-free supplements for skin health and wellbeing. Click on the images to view more details:
Research:
1. Kligman, A.M. and Frosch, P.J., 1979. Steroid addiction. International Journal of Dermatology, 18(1), pp.23-31.2. Rapaport, M.J. and Rapaport, V., 2006. The red skin syndromes: corticosteroid addiction and withdrawal. Expert Review of Dermatology, 1(4), pp.547-561.
3. Hengge, U.R., Ruzicka, T., Schwartz, R.A. and Cork, M.J., 2006. Adverse effects of topical glucocorticosteroids. Journal of the American Academy of Dermatology, 54(1), pp.1-15.
4. Coondoo, A., Phiske, M., Verma, S. and Lahiri, K., 2014. Side-effects of topical steroids: a long overdue revisit. Indian dermatology online journal, 5(4), p.416.
5. Hajar, T., Leshem, Y.A., Hanifin, J.M., Nedorost, S.T., Lio, P.A., Paller, A.S., Block, J. and Simpson, E.L., 2015. A systematic review of topical corticosteroid withdrawal (“steroid addiction”) in patients with atopic dermatitis and other dermatoses. Journal of the American Academy of Dermatology, 72(3), pp.541-549.
6. Fukaya, M., Sato, K., Sato, M., Kimata, H., Fujisawa, S., Dozono, H., Yoshizawa, J. and Minaguchi, S., 2014. Topical steroid addiction in atopic dermatitis. Drug, Healthcare and Patient Safety, 6, p.131.
7. Pampura, A.N., 2005. Prevalence of atopic diseases and the use of topical corticosteroids. Is there any connection?. Medical Hypotheses, 64(3), pp.575-578.
8. Rapaport, M.J. and Rapaport, V.H., 2004. Serum Nitric Oxide Levels in Red Patients: Separating Corticosteroid-Addicted Patients From Those With Chronic Eczema. Archives of Dermatology, 140(8), pp.1013-14.
9. Rapaport, M.J. and Lebwohl, M., 2003. Corticosteroid addiction and withdrawal in the atopic: the red burning skin syndrome. Clinics in Dermatology, 21(3), pp.201-214.
11. Rathi, S.K. and Kumrah, L., 2011. Topical corticosteroid-induced rosacea-like dermatitis: A clinical study of 110 cases. Indian Journal of Dermatology, Venereology, and Leprology, 77(1), p.42.